LACONIA — The 9-month-old coronavirus pandemic has been tiring for people in all walks of life, but especially for nurses who have been saddled with additional responsibilities, cumbersome protective garb and nagging worries about bringing the disease home.
The Laconia Daily Sun spoke with two nurses at Lakes Region General Hospital and two at Speare Memorial Hospital in Plymouth to get an idea of how their jobs have changed in a year in which 15,749 people statewide have tested positive for COVID-19, 822 have been hospitalized and 504 have died.
Rural communities served by the two hospitals have had a better experience with the disease than population centers in the state’s southern tier, according to state Health and Human Services. Grafton County has had 430 cases, 11 hospitalizations and two deaths, while Belknap County has had 461 cases, 16 hospitalizations and seven deaths.
Still, the virus has changed the lives of frontline medical workers everywhere.
Nurse Simpson
Beth Simpson, a registered nurse and director in the med/surg department and birthing suite at Speare, said her day begins by taking an online survey from home to assess the risk that she may be infected.
She must also take her temperature.
“Then when we’re here, we have to wear a mask and eye protection with every patient, all the time,” Simpson said. “Whenever we are anywhere in public areas you have to wear eye protection and a mask.”
The eye protection could be a shield or goggles. Eye glasses, which tend to fog up, can be difficult to deal with at times.
When caring for a patient with COVID-19, nurses also wear a full gown and an N95 face mask. They try to get a lot accomplished in one visit. They don’t want to have to go into and out of a room multiple times if they can avoid it.
“It does take a little thought before you go in a room,” Simpson said. “We also ask the patients to wear a mask while we’re in the room.”
COVID-19 patients can’t receive visitors, so the nurses end up being the main people they see on a daily basis.
“That is really hard,” Simpson said. “We purchased iPads specifically for patients to do Zoom calls or FaceTime. We try to encourage that, so they can see their families.”
Disease uptick
The number of positive test results for COVID-19 has skyrocketed statewide as more people are indoors in colder weather. Fewer than 20 cases were reported some days over the summer, but on Wednesday there were 447 new positive tests, including 24 in Belknap County and 11 in Grafton County.
“There is trepidation,” Simpson said. “We’re still sitting on that fine line now.
“But we feel like we have a good nursing team here that has worked well together. There are lots of challenges, but this small hospital has pulled together with teamwork and work flow input from nurses that have helped us to get through this.”
Day’s end
After a full day at the hospital wearing protective garb, and sometimes caring for people who have the disease, it can be shocking to go into the community and see people unmasked and not socially distanced.
“It’s frustrating,” Simpson said. “We’ve seen that masking does work. I wear one everywhere, except if I’m in my own office, behind a closed door, or at home. I think we should all be paying attention.
“It’s why we are where we are now. People let their guard down a bit.”
Family separation is also difficult.
“I haven’t seen my parents or in-laws for over a year,” Simpson said “They are down in Florida, Thankfully we call and can Zoom, but normally my in-laws are here for most of the summer. They’ve not been able to come up. My parents would also normally come up for Thanksgiving.
“We all have to be careful.”
Nurse Hering
Kristine Hering, the chief nursing officer at Speare, said her nurses are wary.
“We haven't had as much in-hospital Covid as others in the state, but we’re starting to see that change,” Hering said.
Belknap County has 180 current cases, and Grafton County has 160.
COVID-19 patients are labor intensive for nurses. The number of staff members who see these patients are minimized, so nurses often do things like cleaning or lab draws that ordinarily would have been done by someone else.
The result is that nurses end up in a patient’s room for a significant period of time.
“I think the nurses feel that we are doing our best to protect them, but they all have concerns about the possibility of bringing this virus home to their families,” Hering said.
Health care workers account for 2,311, or about 15 percent, of the COVID-19 cases that have been diagnosed in New Hampshire. A total of 62 health care workers have been hospitalized and eight have died.
Success story
A positive note comes when a COVID-19 patient recovers and is discharged.
“It’s incredibly satisfying for the staff, and the feedback we've gotten from patients is absolutely amazing,” Hering said. “They are feeling like the nurses have gone over and beyond to comfort them and educate them and their families, even though contact is limited for family members coming into the hospital.”
She regards education as part of the mission of nursing.
“We do the very best that we can and try to inform people about the science of the disease, facts based on evidence, CDC guidelines. Various scientific organizations give us information that’s credible,” Hering said.
Those who come into the hospital must wear a mask, wash their hands, answer survey questions, practice social distancing.
“If they don't do those things, they can't come in,” Hering said. “There’s got to be protection provided.”
Occasionally, hospital personnel get pushback from people about the need for COVID-19 precautions.
“We don't get much, but we get some,” she said. “Sometimes, patients or visitors will get frustrated.”
She is disappointed with people who don’t believe in taking COVID-19 precautions to protect themselves and others.
“When you are seeing every day people who are really sick, and you yourself are feeling you are put at risk taking care of these patients, it’s disheartening.”
Nurse Leone
At Lakes Region General Hospital, registered nurse Peggy Leone works in pre-surgical testing.
Patients are given a rapid test for COVID-19 as a preliminary to surgical procedures.
“Hopefully, you are testing healthy patients, but some don't know they have symptoms,” Leone said. “Sometimes you do get a positive test. That part of it tends to be nerve wracking. You have concern for your family at home. You think, ‘What am I bringing home to my family?’”
The hospital staff appreciates the community’s support.
One day, police officers formed a heart with their patrol cars in the hospital parking lot. Companies have purchased meals for the hospital staff. People sewed face masks early on and brought them to the hospital.
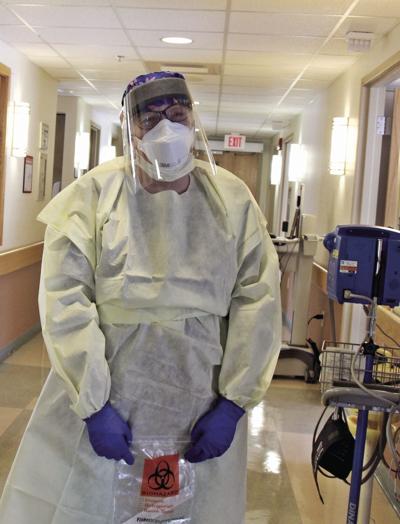
Nurse Stoia
Nancy Stoia, another registered nurse at LRGH, also administers COVID-19 tests.
It’s a drive-up test. She inserts a nasal pharyngael swab in a nostril. The sample is put into its container and then into a biohazard bag. It is then taken away to be tested.
“People tolerate it well,” she said. “Some say, ‘It’s not as bad as I’ve heard.’ Other people aren’t as receptive. It’s not the most comfortable thing, but it’s not too uncomfortable. It’s very brief.”
Stoia has been in nursing for 40 years.
“I’ve taken care of AIDS patients, cancer patients,” she said. “I’ve seen quite a bit, but I haven’t known a pandemic like this.”


















(0) comments
Welcome to the discussion.
Log In
Keep it Clean. Please avoid obscene, vulgar, lewd, racist or sexually-oriented language.
PLEASE TURN OFF YOUR CAPS LOCK.
Don't Threaten. Threats of harming another person will not be tolerated.
Be Truthful. Don't knowingly lie about anyone or anything.
Be Nice. No racism, sexism or any sort of -ism that is degrading to another person.
Be Proactive. Use the 'Report' link on each comment to let us know of abusive posts.
Share with Us. We'd love to hear eyewitness accounts, the history behind an article.