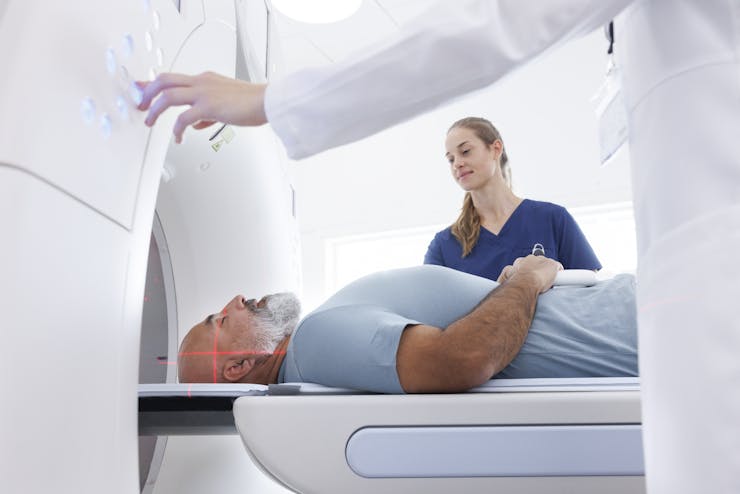
(BLOOMINGTON, INDIANA) Recently, a patient came to the hospital where I work with a persistent cough. Their doctor had ordered a CT scan – a type of imaging that creates detailed cross-sectional pictures of the body’s interior – to look for pneumonia or another infection.
The scan ruled that out, but it also showed something unexpected: calcium buildup in the walls of the coronary arteries. That finding had nothing to do with the cough, but it pointed toward a much more serious problem. After weighing other risk factors, the patient and their doctor decided to start medication to reduce the risk of a heart attack.
Stories like this are becoming more common, and I think about them differently than I used to. I am a cardiothoracic radiologist at Indiana University. In practice, that means I use imaging to diagnose diseases of the heart and lungs. My job is to answer the clinical question in front of me.
But every scan contains far more information than anyone requested, and most of it never gets reported. That is not a failure of any individual radiologist; it is a gap built into how medicine processes imaging data. Closing that gap could matter enormously for patients.
Data hiding in plain sight
A single chest CT produces hundreds of cross-sectional images. Within those images, a trained eye – or an increasingly capable algorithm – can see calcium accumulating in coronary arteries, assess the condition of the muscles along the spine, estimate bone density and detect early changes in the liver. None of this requires an extra scan, radiation or appointment. The information is already there.
This is the idea behind opportunistic screening: using imaging ordered for one purpose to identify other health risks at the same time.
Coronary artery calcium
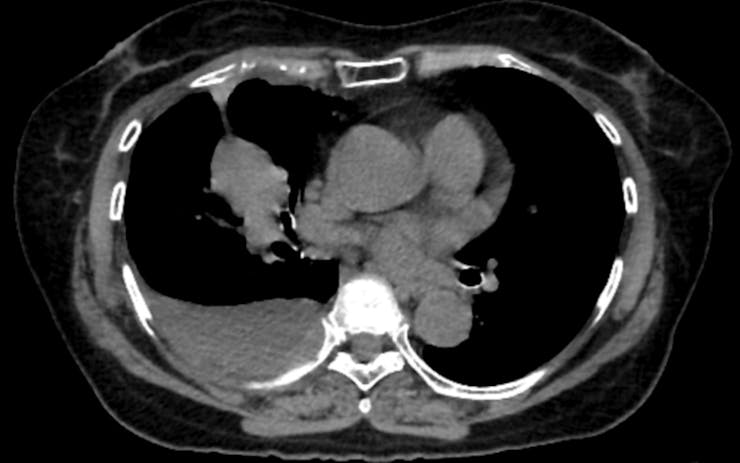
Coronary artery calcium, or CAC, is probably the best demonstration of what opportunistic screening can accomplish. When calcium builds up in the walls of the coronary arteries, it reflects underlying atherosclerosis, the disease process behind most heart attacks. CAC scoring is one of the strongest predictors of future heart attacks, and it adds predictive information beyond what traditional risk calculators provide.
Dedicated cardiac CT scans can measure this calcium precisely. So can a standard lung cancer screening CT, if someone takes the time to look. Studies have found that calcium measurements from lung screening CTs agree closely with those from dedicated cardiac scans, meaning the information is there even when the scan was not designed for cardiac evaluation.
That overlap matters because roughly 19 million noncardiac chest CTs are performed each year in the United States. Every one of those scans passes through the heart. The presence of calcium is visible in the images – yet studies find that when CAC is present, radiologists report it in fewer than half of cases.
The connection runs in both directions. In research my team conducted at Indiana University studying nearly 15,000 patients undergoing dedicated cardiac calcium scans, roughly 1 in 4 were potentially eligible for lung cancer screening, yet fewer than 11% had ever been screened. Patients at risk for heart disease and those at risk for lung cancer overlap substantially, and right now, medicine is not doing enough for either group.
The scale of this missed opportunity becomes clearer when you look at the National Lung Screening Trial, a study that established low-dose CT as an effective lung cancer screening tool. Among participants in that trial, the most common cause of death was not lung cancer. It was cardiovascular disease. More people died of heart attacks than of the cancer the trial was designed to detect.
When high-risk patients are already getting these scans, the question of whether doctors should be doing more with the data becomes hard to ignore.
Other findings worth looking for
Coronary calcium is the proof of concept, but it is not the only finding hiding in these images.
CT scans can measure muscle loss – a condition called sarcopenia – and patients with low muscle mass consistently face higher rates of postoperative complications and death compared with those with normal muscle mass. Bone density from CT predicts fractures related to osteoporosis, and liver fat visible on CT can flag early metabolic disease before a patient has any symptoms. Each of these findings is present in scans already being done, at essentially no added cost.
The point is not to turn every radiology report into a comprehensive evaluation of a patient’s health. It is to capture measurable findings that point toward something treatable, and to make sure that information actually reaches someone who can act on it.
Getting there is difficult. CT protocols vary across institutions, and measurement accuracy depends on how a scan was acquired. Radiology reports are often written in plain prose rather than structured data fields, which is hard to analyze systematically. And extracting data is only half the problem. Using that data in a way that actually changes care requires coordination across radiology, cardiology and primary care that most health systems have not yet built.
Artificial intelligence is beginning to help. Automated tools can now measure bone density, muscle mass, body fat and coronary calcium from routine scans with reasonable accuracy. A study published in March 2026 found that AI analysis of routine mammograms can identify calcium deposits in breast arteries that predict heart attacks and strokes in women. As these tools become more integrated into everyday radiology practice, a scan that answers the question it was asked and also catches something else worth knowing becomes less of an aspiration and more of a realistic near-term goal.
What you can do now
There are practical steps that patients can take while health systems catch up to advances in medical imaging.
If you are undergoing imaging for any reason, it is worth asking your doctor whether the scan showed anything else relevant to your overall health. That question does not always get a full answer, but asking opens a door that otherwise stays closed.
If you are between 50 and 80 with a significant smoking history, you may already qualify for annual lung cancer screening with low-dose CT. Only about 1 in 5 eligible patients are currently being screened. If you have not discussed it with your doctor, bring it up. Cancers found early are far more likely to be cured, and there is good evidence that the same scan can uncover cardiovascular risk that’s worth knowing about.
The mechanic who changes your oil and mentions that your brake pads are worn is not overstepping. He is doing what an attentive, skilled person in his position should do. Opportunistic screening asks whether radiology can be that kind of attentive – not just occasionally and by chance, but routinely and at scale. The data is already there. The only thing missing is the will to use it.
This article is republished from The Conversation, a nonprofit, independent news organization bringing you facts and trustworthy analysis to help you make sense of our complex world. It was written by: Peter Gunderman, Indiana University
Read more:
- Breast density and mammograms: New FDA rule will ensure all women have more information after cancer screenings
- Electronic health records cannot replace a doctor who knows you
- Meet Irene Curie, the Nobel‑winning atomic physicist who changed the course of modern cancer treatment
Peter Gunderman does not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.





















(0) comments
Welcome to the discussion.
Log In
Keep it Clean. Please avoid obscene, vulgar, lewd, racist or sexually-oriented language.
PLEASE TURN OFF YOUR CAPS LOCK.
Don't Threaten. Threats of harming another person will not be tolerated.
Be Truthful. Don't knowingly lie about anyone or anything.
Be Nice. No racism, sexism or any sort of -ism that is degrading to another person.
Be Proactive. Use the 'Report' link on each comment to let us know of abusive posts.
Share with Us. We'd love to hear eyewitness accounts, the history behind an article.